Nasopharyngeal Angiofibroma Juvenile With Subsequent Cerebrovascular Disorder To Therapeutic Embolization: Case Report
Bandes-Vairo M, Medina-Fonseca A, Aldana- Raudales A and Maldonado-Reyes I
DOI10.21767/2572-2107.100013
Bandes-Vairo M1, Medina-Fonseca A2*, Aldana-Raudales A2 and Maldonado-Reyes I2
1Department of Otolaryngology, National Autonomous University of Honduras, Tegucigalpa, Honduras
2Department of Medicine and Surgery, Faculty of Medical Sciences, National Autonomous University of Honduras, Tegucigalpa, Honduras
- *Corresponding Author:
- Medina-Fonseca A
Doctor of Medicine and Surgery, Faculty of Medical Sciences, National Autonomous University of Honduras, Tegucigalpa, Honduras.
Tel: 50422322110
E-mail: medinaalejo@hotmail.com
Received date: July 22, 2016; Accepted date: August 27, 2016; Published date: September 03, 2016
Citation: Bandes-Vairo M, Medina-Fonseca A, Aldana-Raudales A, et al. Nasopharyngeal Angiofibroma Juvenile with Subsequent Cerebrovascular Disorder to Therapeutic Embolization: Case Report. Head Neck Cancer Res. 2016, 1:2.
Abstract
Nasoangiofibroma youth is a highly vascularized tumor almost exclusively male adolescents presentation. 0.5% represents 0.05% of head and neck tumors. Histolgicamente benign but its complex location, a tendency to local invasion, recurrence and aggressive growth makes it peculiar. The nasal obstruction unilateral and later bilateral, unilateral and recurrent epistaxis are frequent symptoms. The diagnosis is clinical, tomographic findings can confirm. Male patient presented with a history of 15 years left nasal obstruction 2 months associated with occasional episodes of epistaxis. Physical exam evidence superomedial mass in the right shoulder moving downward and laterally eyeball, ptosis; anterior rhinoscopy shows vascular mass occluding the left middle meatus 100% of the light. Nasofibrolaryngoscopy denotes vascularized tumor in the left nostril. Sinus tomography reports osteolytic lesion of the left nostril, nasopharynx and pterygopalatine fossa. Magnetic resonance angiography determined occupying lesion in the left nasal region extended to the maxillary sinus and infra-temporal region ipsilateral; in relation to Nasoangiofibroma. Embolization after tumor resection is performed; six hours after showing neurological disorders. Cerebral magnetic resonance angiography revealed acute ischemic event that commits left pre-central region and Post-central; secondary left cerebrovascular event diagnosed embolization. Embolization and endoscopic tumor exercise and left lateral rhinotomy are performed successfully. Biopsy reveals Nasoangiofibroma. As a follow up, nasofibrolaryngoscopy reported recurrent vascular mass, new computed tomography determines osteoma in orbit and frontal sinus on the right side, with extensive skull base injury. Operation was carried nasofibroma with ablation; uncomplicated and good recovery. Evolution provides novel therapeutic methods such as selective embolization useful in reducing complications such as intraoperative bleeding, surgical time and injury to neighboring structures. However, prior to this individualized to assess benefit against risk of these interventions studies are required.
Keywords
Angiofibroma; Nasopharyngeal neoplasms; Therapeutic embolization; Cerebrovascular disorders
Introduction
The juvenile nasopharyngeal angiofibroma (JNA) is a highly vascularized tumor almost exclusively male adolescents presentation [1] (between 14 and 25 years) [2]. However, isolated cases have been reported in men over 25 years and in adolescents [2] women.
They are tumors with a low incidence (1 case per 150,000 inhabitants) [2], representing 0.5% to 0.05% of all head and neck tumors [1].
Although histologically benign, sometimes its complex anatomical location, its tendency to local invasion, recurrence and aggressive growth, make it a sinus tumor with peculiar characteristics [2]. They have slow growth and expand initially within the nasal cavity and nasopharynx and then in the pterigomaxilar pit. Over time, they may eventually erode bone and invade the infratemporal fossa, orbit and middle cranial fossa. The blood supply usually comes from the internal maxillary artery, but can also come from the internal carotid artery or the ascending pharyngeal artery [3].
ANJ the clinic is based on the location, size and extent of the tumor. The initially unilateral and later bilateral, unilateral recurrent epistaxis and nasal obstruction are the most common symptoms [2]. Other signs are dependent on the extension and compression of adjacent structures [1]. Intracranial invasion appears between 10% and 20%, especially in adolescents between 13 and 15 years old. In most of these cases, the tumor has a low probability of spontaneous regression [4].
The diagnosis of this entity can be done basically by clinical data, but the use of imaging studies provide strong support being computed tomography nose and sinuses your choice [5].
The ANJ is a therapeutic problem because of the risk of heavy bleeding and the high rate of recurrence [6]. The treatment of choice for this tumor is surgery [7], with or without preoperative embolization [6]. Later to reduce intra-operative time and degree of surgical difficulty and reducing morbidity and mortality [8].
We present a case of juvenile nasopharyngeal angiofibroma with complications in therapeutic embolization.
Case Report
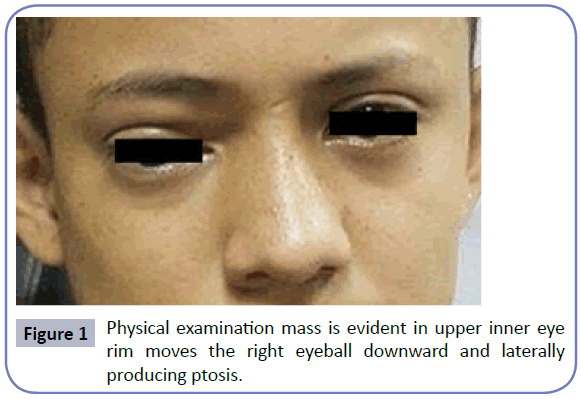
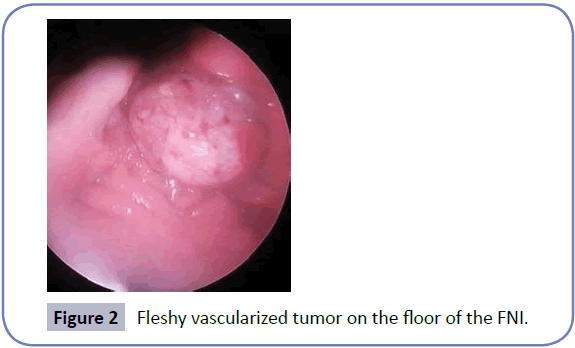
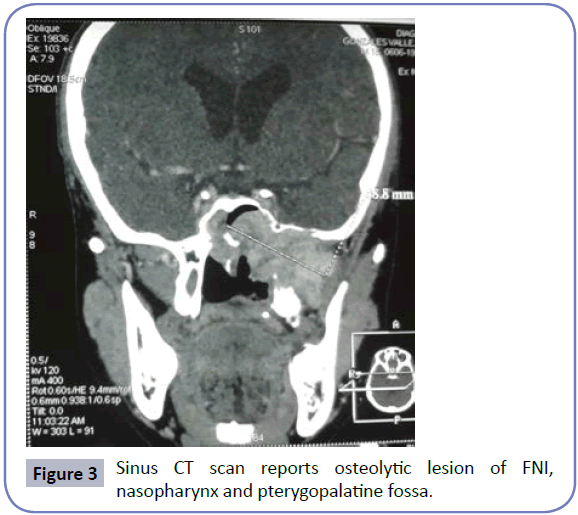
We report the case of male patient of 15 years old from a rural community in the department of Choluteca, Honduras; with a history of nasal obstruction left of 2 months evolution associated with occasional episodes of epistaxis, referred to the otolaryngology service of Hospital Universitario School located in the city of Tegucigalpa, the capital. Physical examination mass is evident in upper inner eye rim moves the right eyeball downward and laterally producing ptosis (Figure 1), the previous rinoscopia whitish mass hyaline smooth appearance is observed, vascular at the left middle meatus occluding 100% of the light from the left nostril (FNI) without epistaxis. Nasofiberoptic evaluation is performed (NFL) denoting fleshy vascularized tumor on the floor of the FNI, septum with deviation to the right, right nostril and free larynx (Figure 2); the rest of the physical examination was normal. Sinus CT scan reports osteolytic lesion of FNI, nasopharynx and pterygopalatine fossa (Figure 3). Angio MRI determines space-occupying lesion that compromises the left nasal region extending to the maxillary sinus and the ipsilateral temporal region infra-presenting heterogeneous strengthening in relation to nasopharyngeal angiofibroma.
It coordinates with interventional radiology service conducting therapeutic embolization prior to tumor resection, left selectively ascending pharyngeal artery and left internal maxillary artery emboli without immediate complications. Six hours after procedure shows altered state of consciousness, right hemiparesis and dysarthria braquio, accompanied by multiple generalized tonic-clonic seizures with oculogiros, drooling, without relaxation of sphincters, about 45 seconds long. Cerebral magnetic resonance angiography demonstrates acute ischemic event that compromises the pre-central region and left Post-central as well as other acute to rostral level in the frontal region and left parietal region punctate ischemic areas, affecting the caudate nucleus. Neurology Service determines diagnosis of secondary embolization left cerebrovascular event and gives management with phenytoin for seizures; physical medicine and rehabilitation management provides for functional recovery.
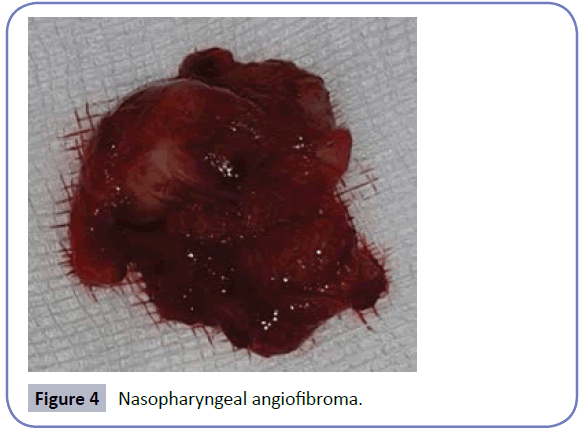
Subsequently new arterial embolization is performed by interventional radiology service and neurovascular n-butyl cyanoacrylate with (NBCA) without complications. It takes 72 hours operating room where post-embolization complete exercise is performed endoscopically and left lateral rhinotomy (Figure 4), a week later post-eoranteriores blockages are removed and cauterized nasopharynx successfully. Biopsy was performed, the study revealed nasopharyngeal angiofibroma.
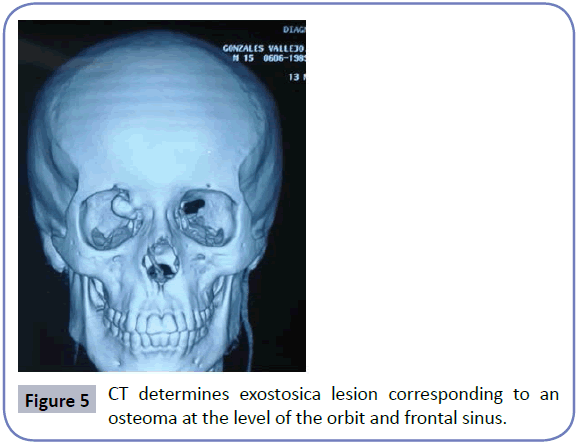
In follow-up evaluations NFL reporting mass of recurrent vascular appearance at the level of the middle turbinate in FNI and their return is decided is carried out. New CT determines exostosica lesion corresponding to an osteoma at the level of the orbit and frontal sinus on the right side, accompanied by extensive tumor lesion of the skull base with affectation orofringe region Pterygopalatine, invading sphenoid sinus and back of ethmoid cells (Figure 5). surgical operation was carried by services otolaryngology and neurosurgery by extension bone and skull base, where ablation nasofibroma performed with posterior packing and after transciliar approach exercise of osteoma more reconstruction medial wall of the orbit, uncomplicated and good recovery.
Discussion
The juvenile nasopharyngeal angiofibroma is a forming tumor vessels in American literature represents 0.05% of head and neck tumors [9]. In Honduras there are no publications on the prevalence of this entity. The typical presentation is in adolescent males (between 14 and 25 years old) [2,9] although it may appear older [9]; in our case it is an adolescent patients 15 years of age, being more frequent gender and age according to data found.
The most common symptoms are nasal obstruction and epistaxis in 56% of cases [2], others related to the tumor, such extension as conductive hearing loss, dacryocystitis, deformity palate, facial palsy, proptosis and bleeding manifestations are described mass [3]. The median time from the onset of these symptoms to patient intervention was 12 months approximately variation between 1 to 60 months [2]. In this case report the patient had left nasal obstruction associated with episodes of occasional epistaxis of 2 months evolution since its inception until the first medical care in a rural area, feeling his mass in upper inner eye rim displacing the eyeball right down and producing lateral ptosis, which makes suspect occupation nostril process of vascular origin.
The diagnosis of ANJ is usually clinical and findings contrasted tomography often establish the diagnosis, showing the nasopharyngeal mass extending to the pterygopalatine fossa in 90% of patients widening the pit and causing anterior bow of the posterior wall of the maxillary sinus. The extension to soft tissue and intracranial commitment are best evaluated using MRI [8]. Here it was evident the space-occupying lesion compromising left nasal region extending to the maxillary sinus, nasopharynx and pterygopalatine fossa in both imaging studies.
The surgical approach and the possibility of combination other therapies, other than surgery, dependent tumor stage. There are different classifications, the most used of Fish and Chandler [10] (Table 1). According to these classifications extension to the maxillary sinus, pterygopalatine fossa and orbit in tracking tomagrafia demonstrate that this case corresponds to Grade IIIa according to Fish and Grade III according to Chandler, because there is no evidence of invasion of cranial cavity.
| Degree | Classification of Fish | Classification Chandler |
|---|---|---|
| I | Limited to the nasopharynx and/or nasal cavity without bone tumor invasion | Tumor located in the nasopharynx. |
| II | Pterigomaxilar tumor invading the pit or the maxillary or ethmoid or sphenoid sinus with bone destruction. | Tumor extends to nasal cavity and/or sphenoid sinus. |
| III | a) Tumor invading the infratemporal fossa or orbit without intracranial invasion. | Tumor extends to one or more of the following structures: maxillary sinus, ethmoid, cleansing pterigomaxilar, infratemporal, orbit and/or cheek. |
| b) With extradural intracranial tumor invasion. | ||
| IV | a) Tumor with intracranial invasion and intracranial extradural without invasion of the optic nerve, the sella or the cavernous sinus. | Tumor invades the cranial cavity. |
| b) Tumor with intracranial extradural and intracranial invasion invasion of the optic nerve or the sella. |
Table 1: Fish and Chandler classification for juvenile nasopharyngeal angiofibroma.
Preoperative arteriography allows us to assess the nutrient vessels and embolization of these vascular lesions, reducing tumor perfusion safely before surgery and intraoperative bleeding even 60% [9,11]. The blood supply comes from the internal maxillary artery, sphenopalatine, ascending pharyngeal and small branches of the internal carotid artery [8]. There may be minor complications in some cases, including fever post-embolization and local pain, headache and lockjaw, depending on the embolized branches [4,8]. The presence of cerebral hemorrhage and tumor-associated embolization is a rare event [11]. In this case left external carotid angiography was performed by observing increased uptake of contrast through the internal maxillary artery and left ascending pharyngeal agreeing with literature. Post-embolization left cerebrovascular event being rare neurological complication secondary to the type of procedure is presented. Clinical data that support the preoperative embolization of hyper-vascularised tumors of the head and neck, especially those bulky, allowing the proper management of these lesions, however there are reports that recommend not embolize due to the relatively high rate of complications. Therefore, careful selection of patients by surgical and endovascular is very important equipment [8].
Various treatments have been proposed although treatment of choice is surgery ANJ for all stages. The purpose of the surgery is complete tumor resection minimize morbidity. The choice of surgical approach should be performed depending on the stage, extension and tumor location. Endoscopic resection of the JNA alone or in combination with limited external approaches is the treatment of choice in the JNA in early stages and at certain centers with sufficient experience ANJ involved in advanced stages [2]. Radiation has also been linked to management for ANJ with intracranial extension in unresectable cases referred by its proximity to the optic nerve and cavernous sinus, when they can carry ophthalmoplegia and possible blindness and when the attempted resection was not complete [1].
Taking biopsy specimens, according to many authors, it is contraindicated because it can cause bleeding; for this reason, histopathology should be excisional. Perform preoperative biopsy or not is still under debate, and there is no consensus to regulate this procedure, since reports have been published incisional biopsy without complications [9].
Recurrence or tumor recurrence is defined as the presence of clinically or radiologically tumor in nasopharynx, nasal cavity or neighboring structures and evidence of growth derived from the onset of symptoms after 6 months of initial treatment [3]. The postoperative tomographic control is necessary for early detection and treatment of recurrences [10]. In the literature, recurrence rates varying between 13% and 50% [3] reported. In the present case evaluation is performed 6 months after surgery showing tumor recurrence with invasion of bone and orbit, demonstrating the high degree of recurrence regardless of the approach performed.
We describe a rare disease in the general population, who despite their benign characteristics is highly invasive making it a potentially deadly tumor. With the evolution in the management of these disease innovative methods such as selective therapeutic embolization useful to decrease complications, intraoperative bleeding, surgical time and risk of injury to neighboring structures are described. This will facilitate and feasible radical resection for surgical equipment; however, individualized pre-intervention clinical trials for evaluating the benefit against the risk of these interventions are required.
Conflicts of Interest
The authors declare no conflicts of interest with the publication of this article.
References
- Hernández VJA, González SH (2011) Juvenile Nasoangiofibroma: an updated review of the diagnosis, classification and treatment. Act of Otolaryngology and Head and Neck Surgery 39: 147-157.
- Llorente JL, Lopez F, Suarez V, Suarez CM (2011) Evolution in the treatment of nasopharyngeal angiofibroma juveniles. Esp Otorrinolaringol Act 62: 279-286.
- Walker K, Muñoz D, Gaete C, Celedon C (2010) Fibroangioma juvenile nasopharyngeal. Experience of 12 years in the Hospital of the University of Chile. Rev Otorrinolaringol Cir Head Neck 70: 17-24.
- Meneses RMN, Avendaño G, Magaña RC, Rodriguez RB, Morales JF (2006) Complications secondary to embolization in nasopharyngeal angiofibroma juvenile. Report on 66 patients. Annals of Mexico Radiology 3: 231-238.
- Chavolla-Magana R, Labra A, Huerta-Delgado AD (2003) Nasopharyngeal angiofibroma juvenile. Meta-analysis of treatment. Rev Med Hosp Gen Mex 66: 71-79.
- Hervas AO, Gregori ES, Vallano LC, Rodero SR, Velázquez A, et al. (2015) Nasopharyngeal angiofibroma juvenile with orbital extension. Arch Ophthalmol Soc Esp 90: 22-25.
- Lora-Diaz FJJ, Jimenez A, Vallejo AM, Malagon FJS, González GIJ (2014) F. Angiofibrona juvenile nasopharyngeal, review of 22 cases. Our experience 2004-2010. Updates in Otolaryngology 1: 9-16.
- Plasencia A, Santillan A, O'Higgins T, Del Pino T, Quiroz K (2015) Endovascular embolization of hypervascular tumors craniofacial. ResearchGate.
- Lamadrid BE, Guerrero-Espinoza D, Gonzalez R, Pliego TAE, Hernandez-Orozco F (2013) Juvenile nasopharyngeal angiofibroma: experience in a general hospital. An Orl Mex 58: 79-86.
- Prayed JF, Saavedra J, Pasache L, Iwaki R, Avello F, et al. (2007) Surgical management of nasopharyngeal angiofibroma juvenile. An Fac Med Lima 68: 254-263.
- Moscote-Salazar LR, Balderrama J, Alvis-Miranda HR, Lee A, Alcalá-Cerra G (2014) Endovascular management of tumors of the skull base. Practical review of the literature. Rev Med Inst Mex Seguro Soc 52: 422-428.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences